No matter how young your daughters are, you can start encouraging good habits such as exercising regularly, maintaining a healthy weight, and eating a healthful diet. Once they become teenagers or young adults, you may wish to let them know about their family history and introduce the idea of genetic counseling and testing. You and your daughters can work with their doctors to determine what’s best in their particular situation.
At the very least, doctors generally recommend regular clinical breast exams starting at age 18. They also can instruct your daughters on how to perform monthly breast self-exams.
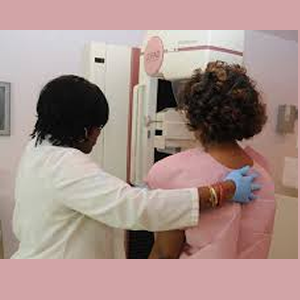
Young women who have inherited a BRCA mutation are advised to start having annual mammograms and MRIs of the breast by age 25. One advantage to having genetic testing information is that young women who test negative for the BRCA mutation do not need to start screening so early. In the absence of genetic testing information, recommendations need to be tailored to the individual, but screening typically begins in the late 20s or early 30s—at least before age 40, which is the usual recommendation for women at average risk.
Some doctors also may prescribe oral contraceptives, which have been shown to reduce ovarian cancer risk. However, since long-term oral contraceptive use may slightly increase breast cancer risk, the pros and cons of this approach need to be discussed on an individual basis.
You can help your daughters by staying up-to-date on the latest research and medical recommendations for women who are considered high-risk. As they grow older, you will be able to help them understand the many options they have.
Reviewed by Jill Stopfer, MS