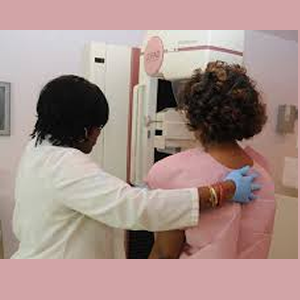
If you choose not to have reconstruction, you will need to see your doctor a few weeks after the surgery to check your incisions and the progress of your healing. If you do have reconstruction, you’re likely to have a series of two or three additional surgeries in the months after mastectomy, followed by office visits to check on your healing. There are different approaches to doing reconstruction, so your exact schedule will depend on the type of surgery you have.
Not all breast cells can be removed with prophylactic mastectomy, so there is still a very small remaining risk for developing breast cancer. You will need to continue seeing your doctor for annual exams.
Reviewed by Jill Stopfer, MS
I have young daughters. Is there anything they should be doing at this point?
No matter how young your daughters are, you can start encouraging good habits such as exercising regularly, maintaining a healthy weight, and eating a healthful diet. Once they become teenagers or young adults, you may wish to let them know about their family history and introduce the idea of genetic counseling and testing. You and your daughters can work with their doctors to determine what’s best in their particular situation.
At the very least, doctors generally recommend regular clinical breast exams starting at age 18. They also can instruct your daughters on how to perform monthly breast self-exams.
Young women who have inherited a BRCA mutation are advised to start having annual mammograms and MRIs of the breast by age 25. One advantage to having genetic testing information is that young women who test negative for the BRCA mutation do not need to start screening so early. In the absence of genetic testing information, recommendations need to be tailored to the individual, but screening typically begins in the late 20s or early 30s—at least before age 40, which is the usual recommendation for women at average risk.
Some doctors also may prescribe oral contraceptives, which have been shown to reduce ovarian cancer risk. However, since long-term oral contraceptive use may slightly increase breast cancer risk, the pros and cons of this approach need to be discussed on an individual basis.
You can help your daughters by staying up-to-date on the latest research and medical recommendations for women who are considered high-risk. As they grow older, you will be able to help them understand the many options they have.
Reviewed by Jill Stopfer, MS
As a woman who is considered high risk, I assume I need to have more than an annual mammogram if I don’t elect to have surgery. What is recommended for women like me?
Doctors generally recommend close surveillance, which is the use of screening tests in an attempt to find cancer at an earlier, and often more curable, stage. Recommendations can vary somewhat depending on your situation, but the general guidelines for women at high risk for breast cancer may include:
- Breast self-exam (BSE) training and regular monthly BSE starting at age 18
- Clinical breast exam (physical examination by a health professional) every six months, starting at age 25
- Annual mammogram and, in some cases, breast MRI (magnetic resonance imaging test). The age and frequency of screening is based on your personal risk assessment.
Although mammography is the standard screening tool for breast cancer, new research suggests that MRI actually may be a better screening tool for high-risk women. One drawback of MRI is that it appears to be more likely to return a false positive result—that is, to detect an apparent abnormality that leads to further testing, only to find it is not breast cancer. However, many experts are now recommending that high-risk women opt for breast cancer screening done with MRI.
You may wish to discuss this possibility with your doctor and find a facility with the expertise and equipment needed to screen for breast cancer in this way. You also should ask if he or she recommends close surveillance for ovarian cancer, which requires having regular blood and imaging tests.
Reviewed by Jill Stopfer, MS
I’ve heard that prophylactic mastectomy (surgical removal of the breasts) is the best way for high-risk women to prevent breast cancer, but it seems so drastic. I also know some women have had prophylactic removal of their ovaries. How greatly do these procedures reduce risk?
Studies suggest that prophylactic mastectomy affords the greatest protection against breast cancer, reducing risk by as much as 90 percent. However, there are disadvantages to be considered, such as the pain and inconvenience of breast removal and potential reconstruction, the scars that can result, and the fact that reconstructed breasts have no sensation and cannot be used to breastfeed. You need to weigh these concerns carefully and arrive at the decision that is right for you. Some women simply are not interested in this surgery, despite being at high-risk for breast cancer.
Women who have inherited risk for ovarian cancer due to a BRCA gene can consider prophylactic oophorectomy, or removal of ovaries. Studies have shown that this procedure can dramatically lower ovarian cancer risk. Because screening for ovarian cancer is not nearly as effective as screening for breast cancer, most centers encourage prophylactic oophorectomy after childbearing is completed and after age 35. There is a very small remaining risk for primary peritoneal carcinoma, an ovarian cancer-like disease that develops in the lining of the abdominal cavity.
Another benefit of prophylactic oophorectomy is that it has been shown to reduce breast cancer risk by at least 50 percent in women who are still pre-menopausal. This reduction occurs because removing the ovaries takes away the body’s main source of the female hormone estrogen, which can fuel breast cancer development. Unlike mastectomy, this surgery preserves the body’s outward appearance, but it also causes menopause in those who have not reached this stage of life already. You could experience sexual side effects such as decreased sex drive and pain during intercourse due to dryness, as well as other symptoms ranging from hot flashes, mood swings, and depression to joint pain and insomnia. There are some long-term health risks as well.
To help with these side effects, some women, especially those who have not had a prior breast cancer diagnosis, elect to take short-term hormone replacement therapy (HRT) until about age 45. Studies suggest that these women still benefit from a reduction in breast cancer risk, since HRT replaces only a fraction of the hormones that the ovaries normally produce. You need to discuss these issues carefully with a provider who has expertise in cancer genetics, so that appropriate decisions can be made for your situation.
Reviewed by Jill Stopfer, MS
Surgery doesn’t seem like the right answer for me. Is there anything else I can do to lower my risk of breast cancer?
Your doctor may prescribe a medication such as tamoxifen or raloxifene, two selective estrogen response modifiers (SERMs) that block the effects of estrogen on breast tissue, which inhibits the cancer development process in some women. In 1998, the Food and Drug Administration approved the use of tamoxifen for reducing the incidence of breast cancer in women with multiple risk factors for the disease. This approval was based on the results of the National Cancer Institute’s Breast Cancer Prevention Trial, which showed that tamoxifen reduced the chance of getting breast cancer by 44 percent. However, the specific impact of tamoxifen on risk in women with BRCA1 and BRCA2 mutations has not yet been studied thoroughly. Risks of tamoxifen include uterine cancer, blood clots, cataracts, and menopausal symptoms.
The SERM raloxifene has been found to reduce breast cancer risk as much as tamoxifen does, but with a lower risk of side effects. However, its impact on BRCA1 and BRCA2-related risk also has not yet been studied thoroughly.
You can discuss these and other options with your doctor, along with the possibility of taking oral contraceptives to lower ovarian cancer risk. You may wish to participate in a clinical trial that is studying different approaches to lowering cancer risk in women like you. A good starting point is the clinical trials section of the National Cancer Institute Web site.
Finally, you can follow the recommendations given to all women for lowering breast cancer risk, such as maintaining a healthy weight, eating a healthful diet rich in fruit and vegetables, exercising regularly, and limiting alcohol intake to no more than one drink per day.
Reviewed by Jill Stopfer, MS
How can I find out where to go for genetic counseling and/or testing, and get more information?
First, talk to your doctor to see what programs might be available in your area. You also may find the following resource helpful:
National Cancer Institute Cancer Genetics Services Directory (800) 4-CANCER
Reviewed by Jill Stopfer, MS
How is genetic testing done?
The test involves giving a small sample of blood that is tested in a lab for the BRCA mutations. Results are generally available in about three to four weeks. You should receive them from your doctor and/or genetic counselor through either a scheduled telephone or in-person appointment, so that all the ramifications of the results for your personal situation can be discussed.
The results are most meaningful if a BRCA mutation has already been confirmed in a relative who had cancer. If at all possible, a sample of his or her blood or tissue should be tested first.
Reviewed by Jill Stopfer, MS
I’m not sure I want to know whether or not I have inherited a BRCA mutation. What are the main advantages and disadvantages of going through with genetic counseling and testing?
The main advantage is knowledge. If you know that the breast and/or ovarian cancer in your family is due to a genetic mutation, and you test negative, you no longer have to worry about being high risk. If you test positive, you can take steps to prevent cancer, such as having surgery or taking medications, or try to catch it early through more frequent screenings starting at a younger age.
There are some disadvantages. You may feel excessively anxious after receiving a positive result. You may not want to have surgery, and you may worry that screening and medications offer no guarantees against getting cancer. The genetic testing process also can cause family strife if members disagree on whether or not it is a good idea. Finally, genetic testing results are not always straightforward, sometimes coming back “indeterminate” or uncertain. This is one reason why it is critical to have your testing arranged by someone who has expertise in cancer genetics.
Your doctor and genetic counselor can help you weigh these and other issues carefully before moving ahead. You also can change your mind at any point in the process. Once results are available, for example, you can choose to delay receiving them until you are ready.
Reviewed by Jill Stopfer, MS
If I do have a BRCA mutation, how does my risk for breast cancer compare to that of an average woman? Am I at risk for any other health conditions?
If you have a BRCA mutation, your lifetime risk of breast cancer ranges from 50 to 85 percent, versus 13 percent for an “average risk” woman. Your risk of ovarian cancer is higher as well, ranging anywhere from 16 to 60 percent, versus just 1-2 percent for the average woman. (The range is due to different findings from different studies, as well as the fact that BRCA1 and BRCA2 are associated with different levels of risk.) In addition, if you have a BRCA mutation, you are more likely to develop these cancers before age 50.
Your genetic counselor can help you better understand your individual level of risk.
Reviewed by Jill Stopfer, MS
Are the so-called “breast cancer genes” (BRCA1 and BRCA2) the only two that increase breast cancer risk? And are they always inherited on the mother’s side?
You can inherit mutations in the genes known as “BRCA1” or “BRCA2” from either your mother’s or your father’s side of the family. Normally, BRCA1 and BRCA2 function as tumor suppressor genes, producing proteins that help repair any damage to your cells’ genetic information and suppress abnormal cell growth. When a BRCA1 or BRCA2 gene has a mutation, or a “misspelling” in the letters of the genetic code, this repair function is usually lost—increasing the risk for breast, ovarian, and some other cancers.
In some families, multiple cases of breast and/or ovarian cancer cannot be traced back to the BRCA1 or BRCA2 genes. Researchers are now searching for other inherited genetic mutations that may be responsible for increased risk.
Regardless of family history, you also may be considered to be at higher-than-average risk for breast cancer if you:
- Had radiation therapy to the chest for treatment of a past cancer
- Have had previous breast biopsies (examination of surgically removed tissue under a microscope) that detected atypical hyperplasia (fast-growing cells)
- Have been diagnosed with ductal carcinoma in situ (DCIS) or lobular carcinoma in situ (LCIS). These conditions are considered to be “pre-cancers” because they stay in place and do not spread to surrounding tissues.
Reviewed by Jill Stopfer, MS